Facet Block (Medial Branch Block)
What is the purpose of this procedure?
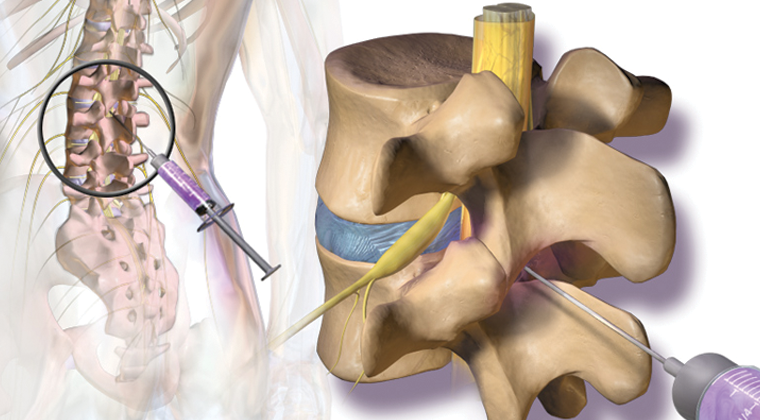
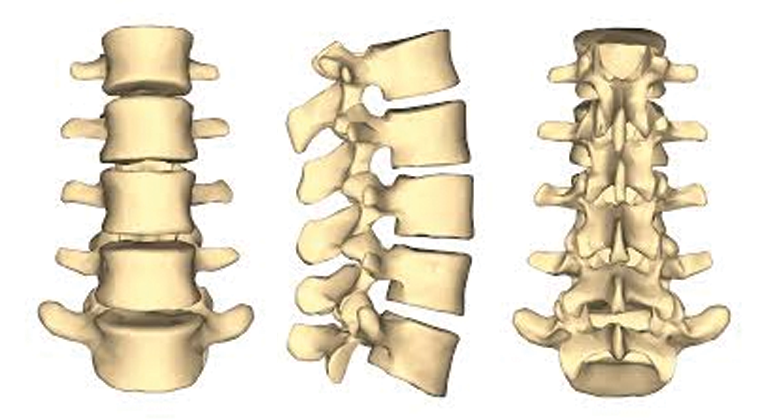
Facet blocks (also known as medial branch blocks) are a diagnostic procedure used to identify and manage a painful facet joint. The facet joints lie between vertebrae in the spine. They allow the spine to bend, flex, and twist. The medial branch nerve carries nociceptive signals from the facet joints. Inflammation (swelling) of the facet joints (arthritis) is a common cause for neck and back pain. A medial branch block uses an injection of local anesthetic to numb the nerve to the joint. You may require multiple injections to identify which joints may be associated with your pain.
What are the risks associated with this procedure?
The risks are infrequent. They include:
• Allergic reaction to medication
• Nerve damage (spinal cord and nerve roots)
• Bleeding and bruising at the injection site
• Infection
• No improvement or worsening of your pain in some cases
• Some additional infrequent risks include puncture of the sac around the spinal cord (dura) and the lung (in the thoracic area)
How should I prepare for the procedure?
• You must have a driver with you at the time of check-in and check-out. Your driver must accompany you to the clinic for your procedure. You can be discharged only to the care of a responsible adult driver 18 years of age or older.
• For injections in the neck do not eat 6 hours before the procedure. Small amounts of clear liquids are ok up to 2 hours before the procedure. If you are a diabetic, be sure to discuss an eating and medication schedule with your doctor.
• You may need to stop taking certain medications several days before the procedure. Please remind the doctor of all prescription and over-the-counter medications you take, including herbal and vitamin supplements. The doctor will tell you if and when you need to discontinue the medications.
• It is very important to tell the doctor if you have asthma or had an allergic reaction to the injected dye for a previous radiology exam (CT scan, angiogram, etc.). An allergic reaction has symptoms such as hives, itchiness, difficulty breathing, or any treatment which required hospital stay. The doctor may prescribe medications for you to take before having the procedure.
• Tell the doctor if you develop a cold, fever, or flu symptoms before your scheduled appointment, or if you have started taking antibiotics for an infection.
• It is important that you have some pain on the day of the procedure (at least 4⁄10) so we can assess if the injection helps your pain. If you take an "as needed" pain medication, you may skip it the morning of your procedure.
• If it turns out you do not have much pain on the day of the procedure, think about calling ahead to reschedule.
What will happen during the procedure?
The procedure is performed on an outpatient basis in a special procedure room equipped with a fluoroscope (x-ray).
- For your safety and comfort when you get to the procedure room you will be connected to monitoring equipment (EKG monitor, blood pressure cuff, and blood oxygen monitoring device), and positioned on your stomach.
- Your back is cleansed with an antiseptic soap and the doctor injects numbing medicine into your skin. This will cause a burning sensation for a few seconds.
- The doctor then directs a small needle (with x-ray guidance) to each level that they feel may be affected.
- After that, the doctor injects a contrast dye to ensure that the medicine spreads to the areas needed.
- Lastly, the doctor will inject numbing medication to those areas. Then you will be taken out to the recovery area.
What should I expect after the procedure?
You will be in the recovery area for 15–20 minutes after the procedure. When you leave the facility you will be asked to do things that would bring about your usual pain. Please do not go home and take a nap. Be active and attempt to trigger your usual pain. This will help doctors determine if the areas injected are the ones causing your pain. You may be given a pain diary to record your response to the procedure. This will help your doctor determine the effectiveness of the injection and how to proceed. Keep in mind that this is a diagnostic procedure (a test to find out where your pain is coming from). If you do experience pain from the procedure, it typically is not expected to last for more than a day.
Prepared by:
Ronald Wasserman, M.D.
1.29.2020
Disclaimer: This document contains information and/or instructional materials developed by Michigan Medicine for the typical patient with your condition. It may include links to online content that was not created by Michigan Medicine and for which Michigan Medicine does not assume responsibility. It does not replace medical advice from your healthcare provider because your experience may differ from that of the typical patient. Talk to your healthcare provider if you have any questions about this document, your condition or your treatment plan. Patient Education by Michigan Medicine is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 3.0 Unported (CC BY-NC-SA 3.0) License. Last Revised 06/2018.